The hormonal edge before menopause
Before midlife, many women show a notable resilience against cardiovascular stress. This durability is closely tied to estrogen, a hormone that exerts wide-ranging effects on blood vessels, inflammation, and cellular repair. When estrogen is abundant, the heart’s protective systems appear more responsive.
Estrogen and ANXA1: a built-in shield
Recent research highlights a compelling duo: estrogen and the protein annexin‑A1 (ANXA1). Estrogen boosts ANXA1 levels, and ANXA1 helps moderate vascular injury by tamping down inflammation and stabilizing vessel function. Together, they create a powerful buffer against hypertension‑related damage.
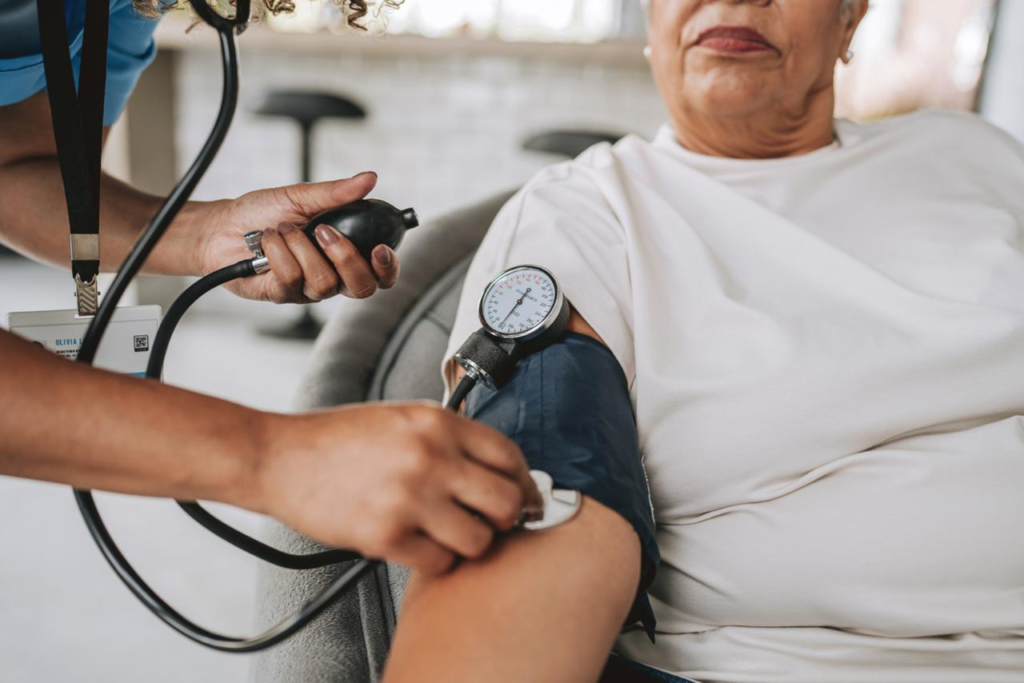
Hot flashes are common during menopause, but the quieter shift is cardiovascular: falling **estrogen** weakens vascular **defenses**, raising risks of **hypertension** and complications. © Fizkes, Shutterstock
Blood pressure, vessels, and inflammation
High blood pressure injures the delicate lining of arteries, inviting inflammation that stiffens the vessels. ANXA1 helps restrain this inflammatory cascade, keeping endothelial cells more stable and less prone to scarring. With estrogen upregulating ANXA1, female vessels stay more compliant under hemodynamic load.
Why the advantage fades after menopause
When estrogen declines, the ANXA1‑mediated brake on inflammation weakens. Arteries become more stiff, blood pressure more labile, and microvascular repair less efficient. The same stress that was once buffered now translates into more overt damage.
From discovery to targeted care
These insights point toward sex‑specific strategies for cardiovascular prevention and therapy. One promising avenue is to mimic or stimulate ANXA1, offering a downstream shield without directly giving hormones. Such an approach could support vascular health after menopause while minimizing hormonal trade‑offs.
Mechanisms behind the female advantage
Multiple, overlapping pathways contribute to this premenopausal edge. Estrogen enhances nitric oxide‑mediated vasodilation, improves mitochondrial efficiency, and modulates immune signaling toward resolution rather than escalation. ANXA1 then consolidates those anti‑inflammatory signals, reinforcing vascular resilience.
What women and clinicians can do now
While drug development evolves, proven lifestyle and clinical steps still matter most. Early detection and tailored management can preserve arterial flexibility and reduce long‑term risk.
- Prioritize regular blood pressure checks and home monitoring.
- Maintain aerobic and resistance exercise to support vascular function.
- Favor diets rich in plants, fiber, and omega‑3 fats to lower systemic inflammation.
- Manage sleep and chronic stress, which elevate sympathetic drive.
- Discuss personalized risk with clinicians, including lipid profile, glucose control, and family history.
Menopause management with nuance
Menopausal hormone therapy (MHT) can relieve severe symptoms, but its cardiovascular role is individualized. The “timing hypothesis” suggests earlier, short‑term MHT may be safer for vascular health than later initiation. Any decision should weigh personal risk factors and shared goals.
A quote to frame the moment
“Understanding how hormones shape vascular defense is not a niche issue; it is central to equitable cardiovascular care.”
Equity in research and care
Women have long been under‑represented in cardiovascular trials, obscuring key differences in disease presentation and drug response. Expanding sex‑aware research improves diagnostics, guides dosing, and refines therapeutic targets for everyone.
How ANXA1 may be leveraged
Therapeutics that amplify ANXA1 signaling could calm endothelial inflammation without full hormonal exposure. By stabilizing vascular barriers and limiting immune over‑activation, such agents might lower hypertensive injury in postmenopausal hearts. Small molecules, peptides, or biologics could activate this pathway with precision dosing.
Beyond the arteries: a systems view
Cardiovascular protection is a whole‑body story, touching kidneys, brain, and metabolic tissues. Estrogen and ANXA1 intersect with autonomic balance, oxidative stress, and extracellular matrix remodeling. Preserving this systems‑level harmony before menopause yields long‑term dividends.
The road ahead
Future trials must test ANXA1‑targeted therapies, define optimal candidates, and track real‑world outcomes. Robust biomarker panels—combining inflammatory, vascular, and metabolic signals—could personalize timing and intensity of care. The goal is simple yet profound: keep vessels flexible, calm inflammation, and protect the heart across a woman’s lifespan.